Acute Appendicitis: Management
- Establish IV access and administer aggressive crystalloid therapy to patients with clinical signs of dehydration or septicemia.
- Administer parenteral analgesic and antiemetic as needed for patient comfort.
- Administer intravenous antibiotics to those with signs of septicemia and to those who are to proceed to laparotomy.
- Patients with a phlegmon or a small abscess: After intravenous (IV) antibiotic therapy, an interval appendectomy can be performed 4-6 weeks later.
- Patients with a larger well-defined abscess: Requires percutaneous drainage and IV antibiotics Interval appendectomy can be performed after the fistula is closed.
- Patients with a multicompartmental abscess: These patients require early surgical drainage.
Antibiotic therapy compared to appendectomy in the treatment of acute appendicitis. Wilms IMHA et al, 2011 Cochrane review
Antibiotics versus placebo for prevention of postoperative infection after appendicectomy. (Review), Andersen BR et a;l, 2009, Cochrane review
Picture below shows a laparoscopic view of inflammed appendix.
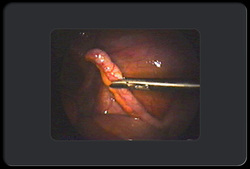
Appendicectomy can be performed by the traditional open technique or laparoscopically.
As with other laparoscopic surgeries, the advantages of laparoscopic approach are:
- decreased pain
- earlier resumption of diet
- decreased length of hospital stay for appendectomy
Complications or risks of appendicectomy
Common early complications include bleeding, surgical site wound infection, intra-abdominal abscess, unrecognized enteric injury (especially with laparoscopic approach), and fistula formation; late complications include incisional hernia and stump appendicitis.
Surgical site infections (SSIs) are determined by the level of intraoperative wound contamination, with rates of infection varying from less than 5% in simple appendicitis with up to 20% in patients with perforations.
In the postoperative period, fluctuating pyrexia, along with worsening diarrhea, may give clues to the formation of intra-abdominal or pelvic abscesses, specifically after gross contamination of the peritoneal cavity. The incidence of intra-abdominal abscesses is increased nearly 3-fold after laparoscopic appendectomy. The diagnosis can be confirmed by either ultrasonography or computed tomography scanning; the treatment consists of radiological drainage, along with continued intravenous antibiotics.
Reference: Laparoscopic versus open surgery for suspected appendicitis. CD001546 [database online]. Cochrane Database Syst Rev: Sauerland S, Lefering R, Neugebauer EA; 2004.
Common early complications include bleeding, surgical site wound infection, intra-abdominal abscess, unrecognized enteric injury (especially with laparoscopic approach), and fistula formation; late complications include incisional hernia and stump appendicitis.
Surgical site infections (SSIs) are determined by the level of intraoperative wound contamination, with rates of infection varying from less than 5% in simple appendicitis with up to 20% in patients with perforations.
In the postoperative period, fluctuating pyrexia, along with worsening diarrhea, may give clues to the formation of intra-abdominal or pelvic abscesses, specifically after gross contamination of the peritoneal cavity. The incidence of intra-abdominal abscesses is increased nearly 3-fold after laparoscopic appendectomy. The diagnosis can be confirmed by either ultrasonography or computed tomography scanning; the treatment consists of radiological drainage, along with continued intravenous antibiotics.
Reference: Laparoscopic versus open surgery for suspected appendicitis. CD001546 [database online]. Cochrane Database Syst Rev: Sauerland S, Lefering R, Neugebauer EA; 2004.